
ΑΙhub.org
Using AI-enhanced music-supported therapy to assist stroke patients

Stroke currently ranks as the second most common cause of death and the second most common cause of disability worldwide. Motor deficits of the upper extremity (hemiparesis) are the most common and debilitating consequences of stroke, affecting around 80% of patients. These deficits limit the accomplishment of daily activities, affect social participation, are the origin of significant emotional distress, and cause profound detrimental effects on quality of life.

Stroke rehabilitation aims to improve and maintain functional ability through restitution, substitution and compensation of functions. The restoration of motor deficits and improvements in motor function typically occurs during the first months following a stroke and therefore, major efforts are devoted to this acute stage. Despite the recommendations for maintaining an active lifestyle, stroke survivors show low levels of activity and they may even experience functional deterioration during the chronic phase. However, numerous studies have found that functionality can be improved with training in chronic stroke patients. In this context, there has been an increasing interest in the rehabilitative potential of music. Music-based therapies have a multisensory nature that fits with rehabilitation principles, they seem enjoyable for patients, and are feasible to apply. One of the most-investigated music-based therapies is music-supported therapy (MST), where patients are trained to play musical instruments to enhance the motor function of the upper extremity.
The goal of the Play&Sing project is to take a step further in MST interventions by developing an AI platform, HMST, to allow home-based MST using previous experience in hospital-based MST interventions to induce upper limb motor recovery.
With HMST, patients perform rhythmic exercises with percussion instruments and play some musical sequences with a keyboard connected to a tablet-based application. HMST increases motivation and patients’ active participation via self-regulated music training at home by incorporating (1) a continuous monitoring of patient activities; (2) prediction and prescription algorithms to personalize exercises, adjusting their difficulty to the patient’s progress and needs; (3) positive feedback and gamification strategies as a mechanism to enhance patient adherence and learning.
The role of the prediction component is to continuously determine the effect of the intervention. To assess such effect, additionally to the patient profile generated from different motor and cognitive tests, three different indicators are exploited to assess the performance of a patient during the training sessions: the execution speed, the key pressure, and the errors.
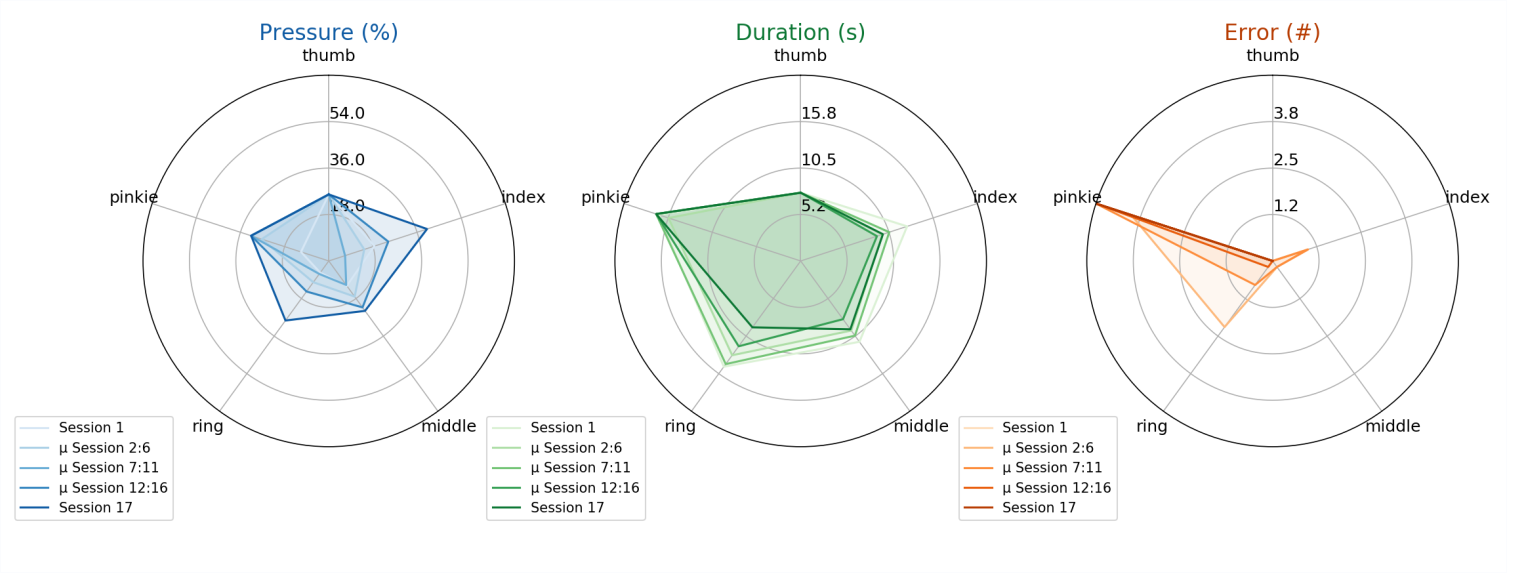
After each patient session, the prediction component, by combining case-based reasoning (CBR) and regression techniques, revises the prediction by incorporating the performance information of the last session.
The role of the prescription component is to propose to each patient the most pertinent activities combining the therapeutic goals prioritized by therapists and the preferences of the patient. The task is modelled as an optimization problem where multiple activities (melodic sequences played with a specific fingering pattern) have to be distributed along several training sessions trying to maximize the value of the intervention, where the value depends on the estimated contribution of each activity. The contribution of each activity is continuously estimated from the analysis of patient performance, the therapeutic goals, the preferences, and the accumulated experience from other patients using the platform.
The prescription component exploits two sources of information: intra-patient information and inter-patient information. The first step is to select a subset of appropriate exercises, i.e. exercises estimated as feasible and not too trivial (e.g. which have been easily overcome previously). This selection is performed by using a CBR system that, measuring clinical and performance similarities, ranks activities according to past experience. The second step is to weigh each activity according to its effectiveness, and intervention values within similar patients. Next, activity weights are refined according to patient preferences and therapist goals. Finally, the list of activities, their associated weights, and intervention constraints (such as the maximum number or repetitions per activity) are sent to the optimiser.
You can find out more about the project here.
tags: Focus on good health and well-being, Focus on UN SDGs










